Overview This hospital serves a rural population with high-acuity needs. Despite its small size, the facility manages a steady volume of emergency and short-term critical care patients, often stabilizing complex cases before transfer to larger regional hospitals.Physicians balance bedside care with documentation responsibilities, and the revenue cycle team is lean. The hospital reached out to […]
Overview A 55-bed community hospital located in the Midwest generates approximately $48M in annual net patient revenue. The hospital serves a mixed rural and suburban population and maintains a payer mix primarily composed of Medicare and regional commercial payers, with a moderate Medicaid presence. The organization initially engaged AnnexMed to support broader revenue cycle optimization […]
Overview This hospital serves a rural population with high-acuity needs. Despite its small size, the facility manages a steady volume of emergency and short-term critical care patients, often stabilizing complex cases before transfer to larger regional hospitals.Physicians balance bedside care with documentation responsibilities, and the revenue cycle team is lean. The hospital reached out to […]
Overview A multi-location dental practice specializing in restorative and implant procedures had experienced steady growth in implant case volumes over recent years. The practice provided a range of advanced services including implant placement, abutment procedures, bone grafting, and final crown restorations. While clinical outcomes remained strong, they began noticing inconsistencies between completed implant treatments and […]
Overview A community trauma center handling 35,000–45,000 emergency encounters each year was struggling to keep trauma charts moving. With only a small coding team, trauma activations and critical care encounters were piling up, and a 4–5 day backlog had become the norm. Important details were being missed, injury specificity, sequencing, and critical care time increments, […]
Overview A mid-sized surgical and outpatient practice was experiencing mounting operational strain as preventable denials and documentation inconsistencies continued to disrupt their revenue cycle. Irregular pre-bill reviews, delayed clarification loops, and uneven modifier usage drove higher rework volumes and elongated reimbursement timelines. These gaps inflated AR, slowed cash visibility, and made month-end close increasingly unpredictable […]
Overview A small but rapidly expanding pain management group in the Midwest, operating with four providers across two clinic locations, was experiencing significant delays in prior authorization processing. Despite using an EHR-integrated workflow, their average turnaround time had stretched to 22 days. High volumes of authorizations for lumbar injections, RFAs, stimulators, advanced imaging, and conservative […]
Client Overview A two-location dermatology practice in Philadelphia was thriving clinically but gradually losing revenue without realizing it. On the surface, claim payments appeared routine and consistent, but a closer look revealed a recurring pattern of payer underpayments across several high-volume CPT codes and procedure bundles. The in-house billing team, already stretched thin managing both […]
What We Saw at the Start A multi-specialty physician group in the southeastern United States, with more than 45 providers across primary care, orthopedics, and cardiology, was in a period of rapid expansion. Over 18 months, the group strengthened its network by acquiring three independent practices. The acquisition promised more revenue and efficiency. However, reality […]
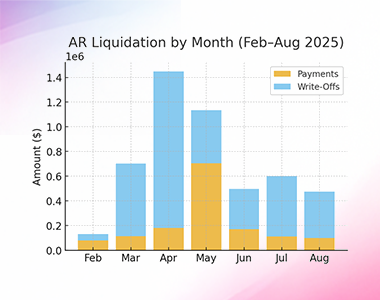
Setting the Stage for Recovery A Utah-based multi-specialty provider faced the complex challenge of liquidating a substantial legacy AR portfolio while maintaining operational efficiency. From February to August 2025, the organization aimed to convert aged receivables into cash, minimize write-offs, and reconcile outstanding credits. At the same time, leadership needed accurate financial forecasts to guide […]