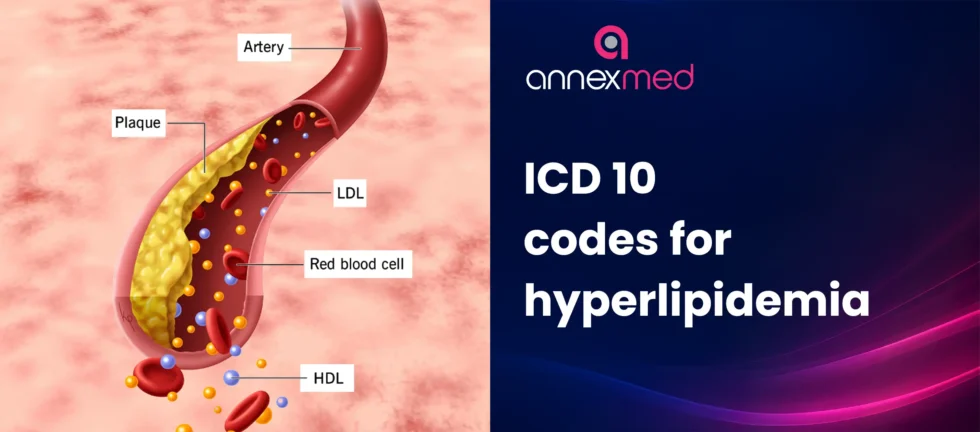
Hyperlipidemia coding is often treated as routine. In practice, it demands precision, clinical awareness, and strict adherence to ICD 10 classification rules.
At the center of this process is one critical requirement: assigning the correct ICD 10 code based on the exact lipid abnormality documented by the provider. Even minor deviations, such as selecting a general code instead of a specific one, can affect claim acceptance, risk adjustment accuracy, and audit outcomes.
This guide focuses on the complete ICD 10 code for hyperlipidemia, how each code should be used, and what distinguishes one classification from another in real-world coding scenarios.
Table of Contents
Complete ICD 10 Code Set for Hyperlipidemia
Hyperlipidemia is classified under the E78 category, which covers disorders of lipoprotein metabolism and other lipid abnormalities.
Each code represents a distinct clinical pattern, not just a variation of the same condition. Understanding these distinctions is essential for accurate coding.
E78.0 – Pure Hypercholesterolemia
This code is used when cholesterol levels are elevated independently, without a concurrent rise in triglycerides.
Subcategories:
- E78.00 – Pure hypercholesterolemia, unspecified
Applied when cholesterol elevation is documented but lacks further classification - E78.01 – Familial hypercholesterolemia
Assigned when the condition is identified as genetic or inherited
Coding Insight:
Familial hypercholesterolemia is clinically significant due to its early onset and higher cardiovascular risk. When explicitly documented, it must always be coded using E78.01, as it reflects a distinct disease process rather than a general lipid abnormality.
E78.1 – Pure Hyperglyceridemia
This code applies when triglyceride levels are elevated without an associated cholesterol increase.
Clinical Inclusions:
- Elevated fasting triglycerides
- Endogenous hyperglyceridemia
- Very-low-density lipoprotein (VLDL) excess
- Fredrickson type IV hyperlipoproteinemia
Coding Insight:
This category is often underutilized because triglyceride-specific diagnoses are not always clearly documented. Coders must rely on explicit provider confirmation rather than interpreting lab results independently.
E78.2 – Mixed Hyperlipidemia
This code represents simultaneous elevation of both cholesterol and triglycerides.
Why It Matters:
Mixed hyperlipidemia is one of the most frequently encountered lipid disorders in clinical practice. Despite its prevalence, it is frequently misclassified when documentation is incomplete or generalized.
Coding Insight:
E78.2 should only be assigned when the provider clearly identifies the condition as mixed. Even if both lipid values are elevated in lab results, coding must follow the documented diagnosis not inferred clinical interpretation.
E78.3 – Hyperchylomicronemia
This code is used for rare lipid metabolism disorders involving extremely high triglyceride levels, typically caused by enzyme deficiencies such as lipoprotein lipase deficiency.
Clinical Context:
- Often presents with severe hypertriglyceridemia
- May be associated with pancreatitis risk
Coding Insight:
Because of its rarity, this code is used infrequently. However, when documented, it must be assigned precisely, as it reflects a significantly different clinical condition compared to common hyperlipidemia types.
E78.4 – Other Hyperlipidemia
This category captures specific lipid abnormalities that do not fall under standard classifications.
Subcategories:
- E78.41 – Elevated lipoprotein(a)
- E78.49 – Other specified hyperlipidemia
Coding Insight:
E78.4 should only be used when the provider documents a defined but non-standard lipid disorder. It is not a fallback for unclear diagnoses and should not replace more specific codes when those are applicable.
E78.5 – Hyperlipidemia, Unspecified
This code is used when hyperlipidemia is documented without identifying the specific type.
Appropriate Use:
- No distinction between cholesterol or triglycerides
- No additional clinical clarification available
Coding Insight:
While valid, this code provides minimal clinical detail. Its use should be limited to situations where no further specificity can be obtained from documentation.
Extended ICD 10 Codes Related to Lipid Disorders
Beyond the primary hyperlipidemia codes, additional classifications within the E78 category provide deeper specificity for certain conditions.
E78.6 – Lipoprotein Deficiency
Used when there is a deficiency in specific lipoproteins, such as HDL or LDL abnormalities.
Coding Insight:
This is not a hyperlipidemia code in the traditional sense, but it is part of the same metabolic classification and may be relevant in complex lipid disorders.
E78.7 – Disorders of Bile Acid and Cholesterol Metabolism
Assigned when there are metabolic abnormalities affecting cholesterol processing, rather than elevated lipid levels alone.
E78.8 – Other Specified Disorders of Lipoprotein Metabolism
Used for clearly defined metabolic conditions that do not fall into other categories.
E78.9 – Disorder of Lipoprotein Metabolism, Unspecified
Applied when a lipid disorder is documented but lacks classification.
Code Selection Principles for Hyperlipidemia
Assigning the correct ICD-10 code requires a structured evaluation of clinical documentation. Each decision point directly impacts coding accuracy.
1. Diagnosis-Driven Coding
The provider’s documented diagnosis determines code selection. Lab values alone are not sufficient for assigning any E78 code.
2. Condition Classification
The code must align with the specific lipid abnormality:
- Cholesterol → E78.0
- Triglycerides → E78.1
- Both → E78.2
3. Specificity Recognition
When documentation includes qualifiers such as “familial” or “elevated lipoprotein(a),” the corresponding detailed code must be selected.
4. Exclusion of Assumptions
Coders must not interpret clinical data beyond what is documented. Even if lab values suggest a mixed disorder, the code must reflect the provider’s wording.
Documentation Requirements for Accurate Code Assignment
For hyperlipidemia coding, documentation must provide sufficient detail to support precise classification.
Required Components:
- Defined Diagnosis Type
Clear identification of the lipid abnormality - Clinical Confirmation
The condition must be confirmed, not suspected - Supporting Clinical Context
Evidence such as lab findings or treatment plans should align with the diagnosis - Current Status
Indication that the condition is active and relevant to the encounter
Each of these elements ensures that the selected ICD-10 code is fully supported and defensible.
Common Errors in ICD 10 Coding for Hyperlipidemia
Errors in hyperlipidemia coding typically stem from misinterpretation or incomplete documentation handling.
1. Coding Without a Documented Diagnosis
Assigning a code based solely on abnormal lipid panels is not compliant.
2. Misclassification of Lipid Type
Using a cholesterol-based code when triglycerides are the primary issue or vice versa results in inaccurate reporting.
3. Missed Use of Specific Codes
Failing to capture familial or mixed conditions leads to loss of clinical detail.
4. Incorrect Category Usage
Using generalized or unrelated codes when a precise E78 classification is available.
Impact of Accurate ICD 10 Coding on Reimbursement
Hyperlipidemia codes play a significant role in establishing medical necessity and supporting treatment plans.
Reimbursement Relevance:
- Justifies lipid testing and monitoring
- Supports long-term medication management
- Aligns diagnosis with cardiovascular risk evaluation
Claims that include well-defined, specific ICD-10 codes are more likely to be processed efficiently and without additional review.
ICD-10 coding for hyperlipidemia is not simply about selecting a code. It involves accurately translating clinical diagnoses into standardized classifications that reflect the patient’s true condition. Each code within the E78 category represents a specific lipid disorder, making it essential to rely on clear provider documentation, carefully classify lipid abnormalities, and strictly follow established coding guidelines.
When applied correctly, these codes enable accurate reimbursement, support clear clinical communication, and ensure reliable healthcare data reporting. Precision in hyperlipidemia coding ultimately aligns clinical intent with financial outcomes, reinforcing both the quality of care and the integrity of revenue processes.
FAQs
1) Can hyperlipidemia be coded based only on abnormal lab results?
No, coding should be based on the provider’s documented diagnosis, not lab values alone.
2) How often should hyperlipidemia be re-coded for a patient?
It should be coded at each encounter where it is evaluated, monitored, or treated.
3) Is hyperlipidemia always considered a chronic condition in coding?
In most cases yes, but it still depends on provider documentation and clinical context.
4) Can multiple hyperlipidemia codes be assigned for the same patient?
Typically no, unless distinct and clearly documented lipid disorders justify separate codes.
5) Does medication use automatically confirm a hyperlipidemia diagnosis?
No, medication alone is not enough; a documented diagnosis is still required.
Improve Hyperlipidemia Coding Accuracy with Expert Support
Reduce errors and avoid unspecified codes with certified experts ensuring precise ICD-10 coding and proper documentation.
Reach Out To Us